Lyme Disease Diagnosis and Treatment
Dr. Shikhman and Neenah, in conjunction with The University of Wisconsin-Madison and Galaxy Diagnostics, publish article in Microbiology Spectrum: Antibodies to Borrelia burgdorferi and Bartonella species in serum and synovial fluid from people with rheumatic diseases.
The results of the study suggest that synovial fluid could be a useful sample for the clinical diagnosis of Lyme disease. Data shows that antibodies to B. burgdorferi, but not Bartonella spp., are more commonly found in synovial fluid than serum of patients with joint effusion. Since Lyme arthritis is a common—and sometimes difficult to diagnose—rheumatic disease, improving diagnostic capabilities is of utmost importance.We see cases of Lyme disease in San Diego everyday. Lyme disease is among the most frequently diagnosed zoonotic tick-borne diseases worldwide. The bacteria that causes lyme disease belongs to the genus Borrelia. There are at least 37 known species, of which 13 are Lyme related including the more recently discovered Borrelia mayonii. Borrelia burgdorferi is the predominant causative agent of Lyme disease in the United States.
Transmission is mainly mediated through the bite of Ixodes ticks. The blacklegged tick (Ixodes scapularis) spreads the disease in the northeastern, mid-Atlantic, and north-central United States. The western blacklegged dear tick (Ixodes pacificus) spreads the disease on the Pacific Coast. The sheep tick (Ixodes ricinu) spreads the disease throughout most of Europe. The taiga tick (Ixodes persulcatus) spreads disease in throughout most of Asia.
In North America, highly endemic areas are the northeastern and north-central United States, though cases have been reported in all states, but Hawaii. Transmission has not been documented in the tropics.
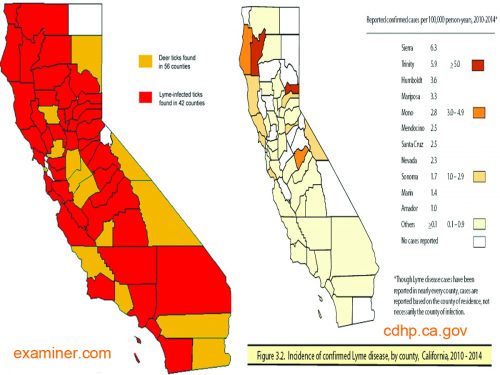
In contrast to common belief, Lyme disease is very common in California. This is a lyme disease map of deer ticks infected with Borrelia burgdorferi in different California counties.
Lyme Disease Transmission
In most cases, the tick must be attached for 36 to 48 hours or more and have taken a blood meal before the Lyme disease bacteria can be transmitted. Most humans are infected through the bites of immature ticks called nymphs as they are smaller and remain undetected for longer. Nymphs are less than 2 mm and start to feed during the spring and summer months. Adult ticks can also transmit Lyme disease, but they are much larger are usually detected before transmission of disease can occur.
Although relatively rare, the transmission of Lyme disease can occur via unprotected sexual intercourse and via vertical transmission from mother to child.
Clinical manifestations
Borrelia are very slow-growing. The incubation period is typically 3–30 days. Borrelia can affect multiple body systems, therefore there is a broad range of Lyme disease symptoms that can be experienced in both acute and chronic infections.
Acute: Approximately 80% of people infected with B. burgdorferi initially develop a characteristic “bull’s eye” rash known as erythema migrans. Erythema migrans usually occurs within 30 days of exposure, at the site of the tick bite and is a circular red, expanding rash, with or without central clearing. Infected individuals may also develop symptoms of Lyme disease including: flu-like symptoms of fatigue, fever, headache, mild stiff neck, joint pains and/or muscle aches.
Subacute: Over days to weeks the infection can spread through the bloodstream to other parts of the body, causing more serious conditions such as meningitis, radiculopathy, facial palsy and myocarditis with atrioventricular heart block.
Chronic: Untreated, infection can progress over a period of months to cause debilitating fatigue, brain fog, tingling and numbness of hands, feet and face, post-exertional muscle weakness, cystic lesions over tendons and ligaments (frequently discovered upon ultrasound examination of the joints), monoarticular or oligoarticular arthritis, peripheral neuropathy, or encephalopathy. These long-term effects of Lyme disease can be observed over months to years.
For more in-depth coverage on how we diagnose and treat Lyme disease visit our other site lymetribune.com
Lyme Diagnosis
The diagnosis of Lyme disease is based on a combination of specific laboratory tests confirming the presence of Borrelia, and clinical symptoms and signs indicative for chronic Lyme disease. Due to the complex immunological and biochemical nature of chronic Lyme disease, the establishment of the actual diagnosis may take several months. In addition, the available genetic testing is frequently utilized to predict a person’s responsiveness to the antibiotic therapy.
From a practical standpoint, the laboratory diagnosis of Lyme disease is based on:
- detection of specific antibodies to Borrelia burgdorferi in the blood or other biological fluids (synovial fluid, cerebrospinal fluid, etc)
- detection of Borrelia burgdorferi specific nucleic acids via PCR (Polymerase-Chain Reaction)
- visualization of Borrelia burgdorferi microbial cells in human tissues (skin, synovial tissue, lymph nodes, blood smears, etc) via specific microscopy
- positive culture of Borrelia burgdorferi isolated from blood and biological fluids – this test is very rarely positive in patients with chronic Lyme disease
Treatment Options for Lyme Disease
We’ve treated hundreds of people with Lyme disease in San Diego. The therapy of chronic Lyme disease is long-term and incorporates the use of oral, injectable or intravenous antibiotics, herbal remedies, food supplements as well as corrective therapies focused on particular Lyme-disease-associated symptoms. Similarly to other chronic infections (tuberculosis, hepatitis C, mycoplasma infection etc), complete eradication of Borrelia is not likely. The practical goal in the therapy of chronic Lyme disease is inducing a dormant state of the disease, where the persisting microorganism is metabolically inactive and does not cause clinically significant symptoms.
Preparing for Treatment: The goal is to eliminate interfering environmental factors such as; heavy metals, immunogenic foods (gluten, dairy products, soy, eggs, corn etc), reduce carb consumption. Address other issues that may be contributing to the symptoms and/or interfere in treatment including; thyroid function, adrenal function and impaired intestinal permeability.
Treatment: The therapeutic response in Lyme is a step-wise one. Initially, the therapy results in improvement of brain fog, followed by the improvement of fatigue and then neurological symptoms and joint pain.
Furthermore, even after successful therapy and induction of the dormant state, a portion of people with chronic Lyme disease deal with asthenia (abnormal physical weakness), which presents in the form of postexertional muscle weakness and fatigue.
The nature of asthenia is typically based on several metabolic abnormalities such as excessive accumulation of lactic acid, depletion of adenosine triphosphate (ATP) the body’s energy source, deviations in urea cycle and accumulation of ammonia, suboptimal production of adrenal hormones, etc. In addition, the central component of asthenia is based on reduction of the nerve-based motor command to working muscles that result in a decline in the force output.
Frequently, Lyme disease is associated with other tick-born infections such as babesiosis, bartonellosis, Rocky Mountain Spotted Fever etc. Therefore, the successful therapy of Lyme disease ideally should incorporate overlapping approaches targeting co-infections as well.
For more in-depth coverage on how we diagnose and treat Lyme disease visit our other site lymetribune.com
Chronic Lyme disease is a treatable disease that requires a multidisciplinary approach, compliance with the therapy and a positive attitude toward the beneficial outcome of therapy. If you are looking for effective treatment for Lyme disease in San Diego, please call us at 858-794-9192
Things to keep in mind:
- Therapy for chronic Lyme disease is not an easy one
- It is a journey through good days and bad days, and even miserable days. In most cases, therapy does not follow a textbook protocol and quite often requires frequent adjustments.
- Be patient and keep a positive attitude and you will be back to a normal life
Preventing Lyme Disease
The best treatment for Lyme disease is prevention:
- Be cautious when walking in the woods, avoiding bushy and grassy areas
- Treat clothing and gear with permethrin prior to your adventures
- Wear light-colored long pants and long-sleeved shirts and wear insect repellent containing DEET on exposed skin
- After walking in wooded areas, thoroughly check the skin for the poppy-seed sized ticks, paying particular attention to the scalp, armpits and groin–remove immediately
